NeuroRestorative Stroke Program: FY21 Residential Rehabilitation Outcomes
NeuroRestorative provides comprehensive rehabilitative treatment for those individuals suffering from the effects of cerebrovascular accidents (e.g., stroke). The program is designed to meet the individualized needs and promotes independence in the home and community. Research completed (Lewis and Horn, 2017; Horn, Lewis, Kincaid & Russell, 2018) revealed the positive effect of NeuroRestorative’s stroke programs for reducing disability from admission to discharge. In addition, stroke recovery tended to have a shorter length of stay and less behavioral disruption than traumatic brain injury rehabilitation.
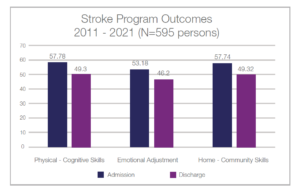
Outcomes are measured using the Mayo Portland Adaptability Inventory Version – 4 (MPAI-4). The MPAI-4 outcome measure is based upon 27 functional items in three areas:
• Abilities (physical, communication, and cognitive functioning).
• Adjustment (emotional, behavioral, social and family functioning).
• Participation (initiation of activities, self-care, home skills, community involvement, and vocational readiness).
**Lower scores represent less disability.
Persons Served Demographics
Program
National Neurorehabilitation Reference
(N = 595)
GENDER
60% Male
40% Female
Average Length of stay
• 94 days.
• Average gain of 8 points by discharge.
Onset of injury to admission
80% had chronicity <6 months duration
Additional Data
• 12% of persons served with stroke required supported care after active rehabilitation.
• 2% of persons served with stroke required neurobehavioral programming.
• 63% returned to a home environment at discharge.
• 6% returned to the hospital for medical complications.
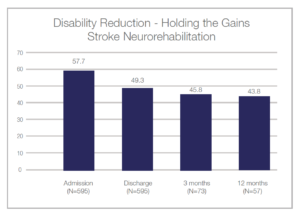
Holding the Gains Following Post-Hospital Rehabilitation:
The gains continued following discharge: 12% of the sample was evaluated at three months and 10% of the sample at 12 months post-discharge. These results show that continued modest reduction and stability of gains was demonstrated at one year. This data indicates that gains achieved in the rehabilitation program continued after discharge.